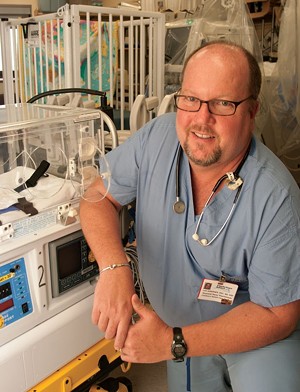
Joe Sorenson
Published May 1, 2012 at 4:00 a.m.
Joseph Sorensen has a very big job working with very small people — about as small as they come.
Sorensen is a neonatal nurse practitioner in the neonatal intensive care unit (NICU) at Vermont Children's Hospital at Fletcher Allen Health Care in Burlington. Sorensen attends difficult deliveries and works with full-term infants born with medical complications.
His specialty, however, is the "littlest of the little." His unit receives the extremely low-birth-weight infants, or babies weighing less than 1000 grams, or 2.2 pounds — that are the result of fewer than 28 weeks of gestation. Not surprisingly, they're among the most complex patients in the hospital.
The state-of-the-art NICU, located on the seventh floor of the McClure Building, is the only one of its kind in Vermont. In the large room, as many as 20 babies at a time can receive care, though the NICU usually has no more than seven or eight in clear plastic isolettes, incubators that protect them from germs, drafts and noise. Others are kept in open beds with overhead warmers. These beds are typically reserved for the most unstable infants. It's a matter of access: If something goes wrong, Sorensen needs to get his hands on them in a hurry.
For obvious reasons, the NICU is an ultra clean environment, and staff and visitors, including parents, must scrub for at least three minutes before entering. In fact, Sorensen says that once these babies go home, they're rarely readmitted to the NICU — even if complications arise.
"Once you've been out in the community," he explains, "you've been exposed to so many things that can really wipe out our littlest of the little who don't have intact immune systems yet."
Despite the stereotype of nurseries being super-quiet, the NICU gets quite noisy at times, due to sounds from ventilators, IV pumps and other life-support equipment.
"We try to keep the noise level down, but I can be the worst offender," Sorensen jokes. "I'm always getting told to shut up!"
A major part of Sorensen's job is transporting newborns to FAHC from other hospitals. His tiny patients may travel from as far away as New York's North Country, Rutland, even parts of New Hampshire. In such cases, Sorensen travels via ambulance as part of a team of five, which includes a nurse and respiratory therapist. "It's a fun part of the job," Sorensen adds. And the ambulance always drives very carefully.
Kids VT caught up with Sorensen on one of his rare days off.
KIDS VT: Help me visualize what a 2.2-pound baby looks like. That's tiny!
JOSEPH SORENSEN: Think of four sticks of butter as a pound. It's kind of [double] that size.
KVT: Does the age and size of preemies keep getting lower?
JS: When I first started there it was very unusual to see a 24- or 25-week gestation infant — you're talking about six months into a pregnancy — come out and survive. Now, it's not unusual for them to survive, and many of them do well. There are some places that are pushing those limits to 23 or 22 weeks. But as you get down into those numbers, you're increasing morbidity, whether it's neurodevelopmental problems, problems with the eyes or cerebral palsy. I think there are limits to what we can do.
KVT: There must be huge challenges in handling babies that small.
JS: Sure. Most of them require ventilators, which means getting breathing tubes into them in the delivery room. They all require some sort of IV access. We can put lines in the arteries and veins in the belly button.
KVT: You must have great manual dexterity.
JS: I'm great at household painting. I always do the corners! But yes, you do develop a lot of manual dexterity starting lines. Intubating is always a challenge, trying to get a breathing tube below the vocal cords.
KVT: Is it a stressful job?
JS: Yeah, but a little bit of stress is always good for everybody. It teaches you that what you're doing is incredibly important. You're working with someone else's child. And all procedures have risks associated with them. I would never become so complacent as to walk in and say, "Oh, this isn't stressful."
KVT: It must be incredibly stressful on the parents, too.
JS: Yes, but we try to offer them as much support as possible. Gone are the days when you would withhold information from parents because you felt it was best to try to protect them.
KVT: What's the hardest part of your job?
JS: It's always hard when you lose a baby. Babies do still die and that's hard. But I think it's important to keep the family involved, so they can start their grieving process.
KVT: What's the most rewarding part?
JS: Sending the kids home with their parents. The baby who probably wouldn't have made it 10 or 15 years ago, to be able to reunite that family and send them home. That and being able to support the family while they're there in the unit, taking these little 25- and 26-weekers with breathing tubes and central lines and having mom put on a breast-feeding gown or dad doing "kangaroo care," where you put the baby right on his chest, cover them with a blanket, kick 'em back in a rocker and let them just hang out.
KVT: Can babies that small breast-feed?
JS: We encourage moms to breast-feed even if the babies can't eat immediately and might not for several weeks or maybe even a month. We also encourage moms to pump and freeze their breast milk because it really is the optimal food for kids. We're trying to get food into them sooner and sooner because it's good for their gut. Everything [in their body] is premature and the only way to overcome that is to get them to grow and heal.
KVT: Are you ever taken aback that you're working on a person that small?
JS: Yeah, sometimes you do a double take and think to yourself, My God, that's really small! But then it's so rewarding to see them come back in one year, two years, three years, 14 years. I've got kids who I took care of when I was a new nurse who are now 25 years old.
KVT: And you remember when they fit in the palm of your hand.
JS: Exactly! We encourage parents to take pictures of that so they'll remember it. Sometimes we'll have moms or dads take off a wedding ring and you can usually fit it up to the baby's wrist on a preemie.
KVT: What's your unit like?
JS: There's tremendous camaraderie. We're all in one big room together and with a lot of the nurses, once they move to the neonatal intensive care unit, they don't go anywhere else. So you work together for years. There's a core group of people up there who I cut my teeth with, and when you're all in one room together, you get to know each of them really well. Sometimes too well! I really enjoy it. You have to love it to work there. Anytime you can wake up in the morning and 98 percent of the time you're happy going to work, you should consider yourself lucky.
This article was originally published in Seven Days' monthly parenting magazine, Kids VT.
More By This Author
Speaking of...
-

Video: Julianna and Sophia Parker of Otter Creek Wildlife Rescue Help Animals — and Humans, Too
Jun 30, 2022 -

Mr. Fix-It: Marty Spaulding Works Behind the Scenes to Help Students Learn on Campus
Aug 24, 2021 -
Back to School During Delta: A Pediatrician With Young Children Offers a Road Map — and Survival Strategies
Aug 24, 2021 -

Can You Dig It? Make Your Own Worm Farm With These Simple Steps
Aug 24, 2021 -

How to Savor Vermont's Shortest, Sweetest Season
Jun 29, 2021 - More »
Comments
Comments are closed.
From 2014-2020, Seven Days allowed readers to comment on all stories posted on our website. While we've appreciated the suggestions and insights, right now Seven Days is prioritizing our core mission — producing high-quality, responsible local journalism — over moderating online debates between readers.
To criticize, correct or praise our reporting, please send us a letter to the editor or send us a tip. We’ll check it out and report the results.
Online comments may return when we have better tech tools for managing them. Thanks for reading.